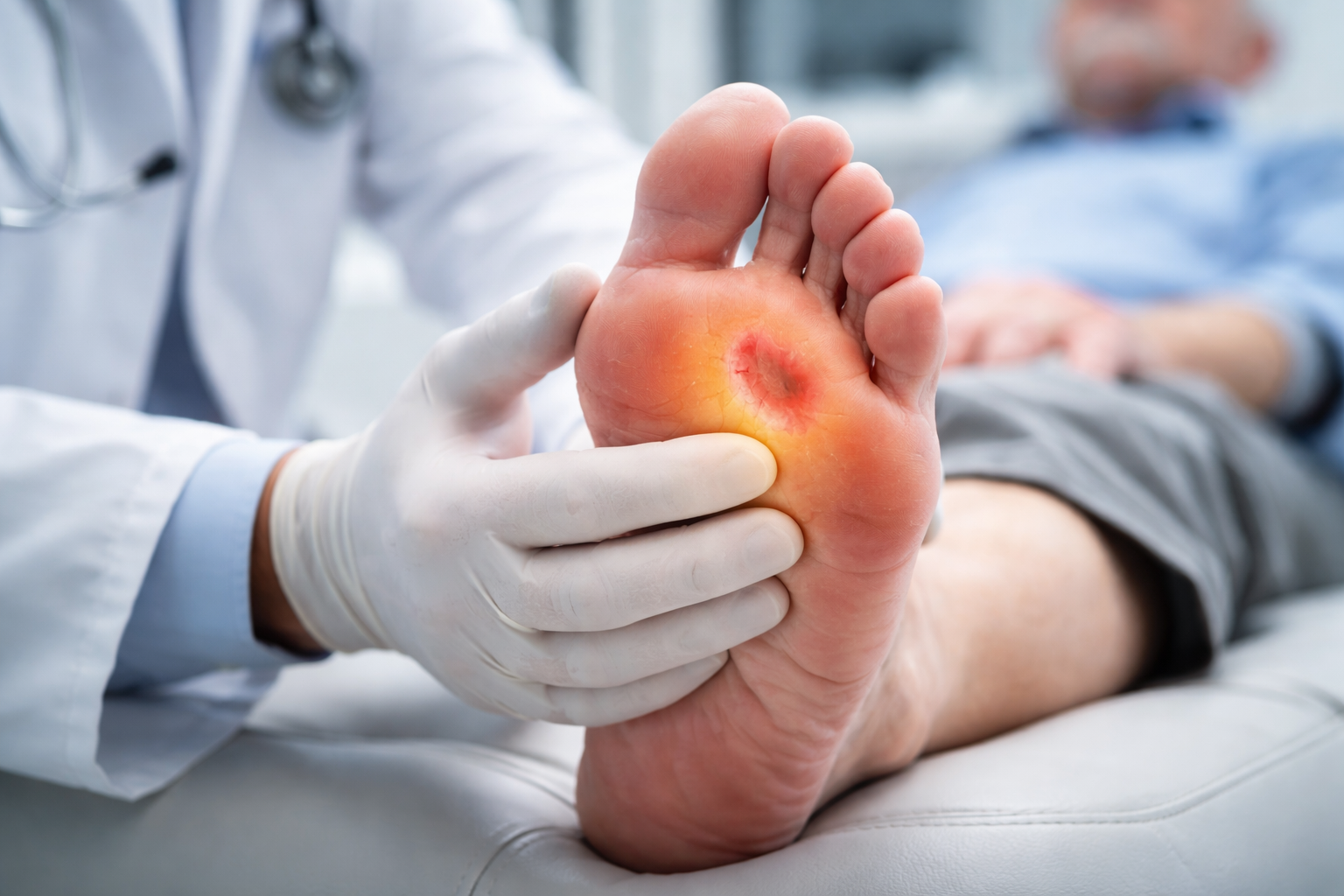
Executive Summary
Every thirty seconds, someone in the world loses a limb to diabetes. There are between 75,000 and 100,000 in the US alone. That is with the best healthcare in the world.
Here’s what we’re dealing with, roughly 37 million Americans have diabetes, and one in four will develop a diabetic foot ulcer at some point in their life. But here’s the thing that really concerns me as a practicing podiatrist, 85% of lower-limb amputations in diabetic patients start with a foot ulcer. While it plays a large role, the is not vascular disease alone. Not neuropathy alone. It’s the infection that pushes patients over the edge.
The gap I see in clinical practice is that we’re great at treating infections once they’ve started. We’ve got antibiotics, we’ve got debridement protocols, we’ve got hyperbaric oxygen therapy when things get serious. But prevention? Actual reduction of the microbial load on the foot before an ulcer even becomes infected? That’s where we fall short. Most patients and their physicians manage their feet the same way they always have, basic hygiene, maybe some foot cream. However, every minute of every day, bacteria and fungi multiply silently in a warm, moist environment, think what is going on in the shoes when they are worn.
VivoThreads’ copper-embedded socks represent something different. This isn’t another topical cream that you apply and forget about. This is a patented textile technology with copper embedded directly into natural fibers. The result is a continuous antimicrobial action attacks pathogens where they’re most likely to colonize-inside the sock, on the skin surface of the foot, in the microenvironment where infection starts.
In my initial clinical experience with three diabetic patients at WeTreatFeet Podiatry (all with current or prior foot wounds), I saw 100% positive response. They reported better comfort, genuine patient satisfaction, and what appeared to be improved clinical markers. That’s not a large sample, but in my 25 years of practice, early signals like this usually mean something. When patients tell me a product “feels really good” and they’re actually wearing it, think of the difference. That’s compliance. And compliance is everything in diabetic foot care.
This white paper examines the clinical imperative for infection prevention in diabetic foot management, the technology behind VivoThreads’ patented copper-fiber innovation, and preliminary observations suggesting that non-pharmacological textile-based antimicrobial strategies merit serious consideration in preventative podiatric practice.
I. The Clinical Imperative: Why Diabetic Foot Health Matters Now
The Scale of the Problem
Let’s start with numbers, because they tell the story of why I’m writing this.
- 75,000+ amputations per year in the United States alone are performed on people with diabetes. Not trauma-related. Diabetes-related.
- 60% of all non-traumatic amputations in this country happen to diabetic patients.
- Every 3.5 minutes, someone loses a limb due to diabetic complications.
- <25% lifetime risk: One out of every four people diagnosed with diabetes will develop a foot ulcer before they die.
- More than 1.5M Americans develop diabetic foot ulcers each year
And here’s the most stark statistic: 37% of patients who undergo a diabetic foot amputation will face a second amputation within five years. Even after we’ve removed the diseased tissue, even after the trauma of surgery, patients lose the other limb. That tells me we’re not actually solving the underlying problem:we’re being reactive instead of preventative.
Why the Foot Becomes a Problem Zone
The foot is unique. It’s at the end of the vascular supply chain, it bears all the pressure and friction from walking. And it lives inside a hot, moist environment most of the day. It becomes the perfect storm for infection.
Here’s what happens physiologically:
Neuropathy (nerve damage from high blood sugar over years) affects 60-70% of people with diabetes. Most don’t even know they have it until they develop an ulcer. Patients lose pain sensation, so a blister, a small cut between the toes, pressure from a shoe doesn’t hurt. The brain never gets the alarm, as someone pulled out the cord! The injury then gets worse.
The microenvironment is hostile. The foot sweats, it’s warm (sustained temperature around 97°F in a shoe), it’s moist. The ideal environment for bacteria and fungi. Staphylococcus aureus loves that. Candida loves that. These pathogens are not just surviving, in this environment, they’re thriving.
Vascular insufficiency compounds the problem. Poor blood flow means lower oxygen delivery to tissues and reduced ability of white blood cells to fight infection. In my practice, I have seen many “minor” foot infection that spirals into sepsis because they didn’t have the circulation to mount an immune response.
Add microbial infection, and you’ve got a situation where:
- The neuropathic patient doesn’t feel the wound getting worse
- The bacteria or fungi (often polymicrobial ormultiple organisms) colonize the site
- Poor circulation limits systemic antibiotic penetration and immune response
- Within 30 days, an ulcer is significantly more likely to be infected
- From there, you’re looking at possible osteomyelitis (bone infection), leading to potential amputation
I’ve operated on enough gangrenous feet to know: once the infection takes hold, the clock starts running.
The Cost of Inaction
We talk about this in practice management too. The financial toll is massive, with over $11 billion spent annually to care for diabetic foot ulcers in the U.S. This is all due to prevention opportunities we’re missing, and money we could save by keeping patients’ feet healthy.
But the human cost is what really matters. The 5-year mortality rate for someone with a major amputation exceeds 70%. Amputation is often framed as saving the life by sacrificing the limb, but the reality is that patient’s quality of life, independence, and longevity all suffer. I have patients who’ve adjusted beautifully to prosthetics, and it is a reminder how impressively the human resilience thrives. Most people, however, would trade anything to have prevented that first amputation.
II. VivoThreads: A Patented Antimicrobial Innovation
The Technology: Copper Embedded in Natural Fibers
VivoThreads holds a patented process for embedding copper directly within natural textile fibers. This isn’t a surface coating that washes away or a chemical applied after manufacturing. It’s copper integrated directly into the fiber itself during production, which means the antimicrobial effect is durable across multiple wash cycles. The data shows effectiveness is maintained even after 50-60 launderings.
Why copper? Because the mechanism of action is elegant and, frankly, hard for pathogens to resist.
The Antimicrobial Mechanism
Copper works through what researchers call a multimodal mechanism. This is what happens with the copper attacks bacteria and fungi in multiple ways simultaneously. This is critical because pathogens can develop resistance to single-mechanism antibiotics. Pathogens can’t easily develop resistance to something that kills them through several different pathways at once.
Here’s what actually happens at the microbial level:
Copper ions released from the fiber interact directly with bacterial cell proteins and enzymes. These proteins are essential for the microbe to breathe, to reproduce, to transfer genetic information. Once copper disrupts them, the microbe’s essential functions shut down. Additionally, copper damages the cell membrane itself.It triggers lipid peroxidation, basically poking holes in the membrane barrier. The cell leaks and dies.
The speed is remarkable. According to recent clinical data presented by Dr. Maggie Thieman at West Virginia University Health System (who is also medical director for VivoThreads):
- Within 30 minutes: 2-3 log reduction (99-99.9% reduction) in common pathogens
- Within 2 hours: Greater than 4-log reduction (>99.99%) in MRSA, vancomycin-resistant enterococci, and Clostridioides difficile
- By 4 hours: Near-complete kill
That’s not slow-acting antimicrobial activity. That’s immediate.
And critically,the effect persists between washes. You’re not relying on a topical cream that you apply daily or a spray that lasts a few hours. Put on the socks. Go about your day. The copper keeps working. As Dr. Michael Schmidt, microibioligist at Medical University of South Carolina said, “It works the day you put it down (on) until you take it out of service.”
Effectiveness Against Relevant Pathogens
In my diabetic foot patient population, the bugs I worry about most are:
- Staphylococcus aureus (including MRSA): The most common pathogen in diabetic foot infections. Copper shows excellent effectiveness.
- Pseudomonas aeruginosa: A gram-negative organism that loves wet environments and often colonizes foot maceration areas. Copper handles this.
- Candida albicans: Fungal infections are common in the diabetic foot, especially in toe web spaces. Copper is effective against fungal pathogens too.
- Gram-negative organisms (E. coli, Klebsiella): Present in 50-60% of moderate to severe diabetic foot infections. Studies confirm copper’s broad-spectrum activity.
One research group tested copper-embedded fabrics and demonstrated:
- 99% efficiency against E. coli
- 99.6% growth inhibition against C. xerosis (a common foot colonizer)
- 99.2% reduction in M. luteus (another odor-causing foot bacterium)
And in vitro testing confirmed: no cytotoxicity to human skin cells. It kills the bacteria; it doesn’t harm the patient’s tissue.
Comfort and Compliance
Here’s something I learned early in my career, the best treatment in the world doesn’t work if patients won’t use it. Compliance is the silent killer in diabetic foot management.
A patient can be prescribed the most expensive prescription shoe, the most sophisticated topical cream, the most effective oral medication. But if it’s uncomfortable, if it feels weird on the foot (ironic when they can’t feet the wound), or if it gets in the way of their normal life, they stop using it. I’ve seen it more times than I can count.
One of the concerns I had before trialing VivoThreads was whether copper-embedded fibers would feel rough, stiff, or “medicinal” in a way that would bother patients.
The socks feel like quality athletic socks. I tried them myself. The copper is embedded in fine, soft natural fibers. They’re not rigid. They’re not uncomfortable. One patient told me they “feel really good,” which is the exact kind of feedback that predicts long-term compliance.
That matters clinically. A sock that prevents 99% of microbial growth but that the patient refuses to wear because it’s uncomfortable is useless. A comfortable sock that is also beneficial, and the patient loves wearing is far more valuable in real-world diabetic foot care. Vivothreads socks has the best of both worlds. Effective and comfortable!
III. Clinical Observations: Initial Patient Experience at WeTreatFeet Podiatry
Study Population and Context
Over a three-month period, I introduced VivoThreads copper-embedded socks to three diabetic patients at WeTreatFeet Podiatry who met specific criteria:
- Type 2 diabetes with established diabetic neuropathy
- Prior diabetic foot ulcers and a documented history of ulceration with healed scars
- Moderate-to-high risk for recurrent ulceration
- None had active osteomyelitis or severe vascular insufficiency
These weren’t theoretical patients. These were people I see regularly, whose foot histories I know well, whom I follow closely.
Clinical Observations
Patient 1: 62-year-old with a history of medial forefoot ulceration (now healed but scarred). Significant neuropathy with difficulty sensing pressure. Moderate peripheral vascular disease. Previous struggles with compliance in shoe and sock gear.
Experience: Wore VivoThreads for4 weeks with follow-up assessments at 2, 4 and 6 weeks. Subjective improvement in foot comfort. No recurrent ulceration. Most importantly, he kept wearing them. “They don’t feel like medical socks,” he told me. Compliance was dramatically better than with previous preventative products I’d recommended.
Patient 2: 56-year-old with current small plantar ulcer (Wagner Grade 1, non-infected at time of sock introduction). Diabetes for 12 years, significant neuropathy. High risk due to a previous deep foot infection requiring IV antibiotics and digital amputation.
Experience: Socks worn in combination with standard offloading and wound care protocol. Ulcer healed within 3. What was notable: no clinical signs of infection developed during the healing period, despite the patient’s high-risk profile. Post-healing, patient continued wearing socks as preventative measure. At 6-week follow-up, no recurrence. Importantly, the socks washed well and no issues related to drainage were noted.
Patient 3: 68-year-old with chronic interdigital (toe-web) maceration and recurrent fungal infection. Multiple topical antifungal treatments had provided only temporary relief. The moisture and warmth in that space just kept feeding the problem.
Experience: Copper-embedded socks introduced with instruction to wear during the day, dry thoroughly between toes before bed. By week 3, maceration visibly improved. By week 6, no active fungal colonization (assessed clinically, no culture obtained). Patient’s own assessment: “My feet feel cleaner.”
What the Observations Suggest
clearly, three patients are not a clinical trial. It’s not a randomized controlled study. It’s not statistically powered evidence. In academic medicine, these are called “case observations,” and they’re at the bottom of the evidence pyramid.
But in clinical practice, case observations matter. It provides information about whether something is worth investigating further. It tells you whether a patient population tolerates an intervention. It provides evidence on whether the mechanism you expect (copper killing bacteria) actually translates to real-world improvements.
What I observed:
- Patient compliance was excellent. No patient reported discomfort. All continued using the socks beyond the trial period voluntarily.
- No adverse events. No dermatitis, no complaints of irritation, no unexpected reactions.
- Clinical markers appeared favorable. No new infections developed. Healing proceeded normally. One patient’s chronic fungal issue (usually recurrent) appeared to resolve.
- Patient satisfaction was genuine. Not the polite satisfaction of someone trying to please their doctor. These patients actually liked the socks.
The positive signal is there. Whether it holds up in a larger, more rigorous study? That’s the next question.
IV. The Role of Preventative Textiles in Diabetic Foot Management
Paradigm Shift: From Reactive to Preventative
Here’s what frustrates me about current standard care: we’re mostly reactive.
Patient comes in with an ulcer; We clean it, culture it, start antibiotics. Infection develops: We escalate to hospitalization, IV therapy, and aggressive operative debridement as needed. Bone involvement: we’re talking amputation risk. We’re good at each of these steps (well, most of us), but we’re always responding after the damage has started and not proactively working to prevent the deterioration.
What if we shifted some of our energy upstream?
The research is clear on one thing: multidisciplinary preventative foot care reduces amputation rates. Studies show that systematic foot assessment, foot care counseling, appropriate footwear, and regular monitoring can meaningfully reduce infection rates and amputation risk. We know prevention works.
The challenge is that current preventative strategies are mostly behavioral. We educate patients on daily foot checks, proper hygiene, good footwear, glucose control. Those are essential, but they require patient compliance and vigilance. Realistically, patients don’t understand or forget 90% of what I told them by the time they reach the door. Education alone doesn’t directly reduce microbial load. Changing habits is very difficult if not impossible.
An antimicrobial textile, something the patient simply wears, something that works continuously without additional effort, something they don’t have to “apply” or “remember”—represents a different approach. It’s a passive antimicrobial intervention. The copper is working whether the patient is perfect with their hygiene or not. It’s there, actively reducing pathogens, as a baseline layer of protection.
Where Copper-Embedded Socks Fit in the Prevention Protocol
In my practice, I think about diabetic foot care in tiers:
Tier 1: Universal measures (applies to all diabetic patients)
- Annual foot examination (or every visit for high-risk patients)
- Glucose control
- Foot care education (daily inspection, proper hygiene, avoiding barefoot walking)
- Appropriate footwear
- Skin integrity management
- Compression if indicated
Tier 2: Enhanced measures (for at-risk patients: neuropathy, history of ulcers, vascular insufficiency)
- More frequent examinations (every 3 months minimum)
- Prescription footwear/orthotics
- Callus debridement, high risk foot care
- Moisture management
- Antimicrobial preventative measures
Tier 3: Aggressive measures (for very high-risk patients: prior amputation, active wounds, severe neuropathy)
- Multi-specialist collaboration
- Advanced wound care (negative pressure, growth factors as indicated)
- Vascular intervention if appropriate
- Careful monitoring for infection
Copper-embedded antimicrobial socks fit naturally into Tier 2 and Tier 3 as a low-risk, high-benefit adjunct to prevent infection. This is not a replacement for any of these measures. It should be treated as an additional and an enhancement to the care of these patients.
In my practice now, I’m considering recommending VivoThreads to:
- Any patient with neuropathy and prior ulcer history
- Any patient with active or recent wounds
- Any patient with interdigital maceration or chronic fungal issues (the copper works against fungi too)
- Frankly, any high-risk diabetic patient where the cost-benefit is favorable
Research Gaps and Future Directions
For this to be successful, we need more evidence. Three patient observations in a single practice is not sufficient evidence.
What I’d like to see:
- A formal randomized trial: Diabetic patients with neuropathy, randomized to copper-embedded socks vs. standard socks, measured for ulcer development, infection incidence, and patient-reported outcomes over 12 months.
- Specific patient populations: Separate analyses for subgroups, active ulcer patients, healed-ulcer patients, foot-maceration patients. This is to determine where copper socks provide the most benefit.
- Cost-effectiveness analysis: What’s the cost per amputation prevented? In health economics, this is vital.
- Mechanism validation in vivo: We know copper kills bacteria in vitro and in experimental textile models. Proof that it’s actively reducing bacterial load on actual human feet in socks would strengthen the evidence base significantly.
V. Conclusion: Why Podiatrists Should Consider Copper-Embedded Antimicrobial Socks
Here is my position: I’m a podiatrist who spends his days treating diabetic foot complications. I’ve performed amputations I wish I could have prevented. I’ve seen the impact on patients’ lives and families. And I’m always looking for legitimate tools that might reduce that burden.
VivoThreads’ copper-embedded socks represent something valuable: a non-pharmacological, passive antimicrobial intervention that addresses a real problem—microbial load on the diabetic foot—with a mechanism that’s scientifically sound and a preliminary clinical signal that’s genuinely promising.
The Case for Clinical Adoption
The need is clear. Every 30 seconds, someone loses a limb to diabetes. Most of those amputations are preceded by foot ulcers that became infected. Prevention is critical.
The technology is sound. Copper’s antimicrobial mechanism is well-established, multimodal (hard to develop resistance), and effective against the pathogens we care about most—Staph. aureus, Pseudomonas, Candida. The patent-protected embedding process ensures durability across multiple wash cycles. The breakthrough of embedding the copper in cotton, an open fiber, as opposed to the traditional polyester based use, is a game changer.
The patient experience is positive. In my three-patient observation, compliance was excellent, patient satisfaction was genuine, and no adverse events occurred. When diabetic patients actually enjoy wearing a preventative sock? That’s not a small thing. That predicts real-world adherence.
The fit in practice is natural. This isn’t a device that requires patient education or special protocols. It goes on like a regular sock. It works continuously. It fits into existing preventative care frameworks without additional burden on the practice.
A Call to Action for Podiatric Colleagues
If you’re reading this, you have experience managing, or want to learn more about diabetic foot complications. The statistics are stark, and the outcomes keep me up at night. It has been established that prevention is dramatically underutilized.
I’d encourage you to consider:
- Trial a product. Test VivoThreads with your own high-risk patients. Observe their response. See whether compliance improves compared to other preventative measures. You don’t need a formal study to gather clinical impressions.
- Educate your team. If the mechanism makes sense to you, talk about it with your nursing staff and clinical team. Preventative mindset has to be team-wide.
- Adjust your counseling. For patients at risk, consider recommending copper-embedded socks as part of your preventative protocol alongside footwear, glucose control, and regular monitoring.
- Document and observe. Keep track of ulcer incidence, infection rates, and patient satisfaction in patients using the socks versus those who don’t. Over time, real-world effectiveness data accumulates.
- Support future research. If a formal study is proposed, consider participating. The evidence base strengthens when multiple practices contribute data.
The Bigger Picture
We talk a lot in podiatry about “limb preservation.” It’s the banner we fly. But if limb preservation starts in an operating room, it is too late. It needs to start in the office or clinic. It starts with preventative strategies that actually reduce the microbial load that leads to infection, which leads to amputation.
Copper-embedded antimicrobial socks won’t solve the diabetic foot problem alone. Patients still need glucose control. They still need proper footwear. They still need regular monitoring. They still need us.
But as one additional, evidence-based, patient-friendly tool in our preventative arsenal? This has merit. Real clinical merit.
I’ve seen the preliminary signal. The technology is sound. The patient experience is good. I think it’s worth bringing into practice. However, I think it’s worth studying more rigorously to prove what preliminary observations suggest. Basically, it is a simple innovation (like copper-embedded socks) that can help us move the needle and keep our patients’ feet healthy and their limbs intact.
References
[1] Azura Vascular Care. Statistics About Amputation Due to Diabetes and Foot Ulcers. Retrieved from https://www.azuravascularcare.com/infopad/diabetic-foot-amputation-stats/
[2] Infection Control Today. (2025, December 1). Copper-embedded textiles show promise in reducing microbial burden and supporting infection control. https://www.infectioncontroltoday.com
[3] Lipsky, B. A., Berendt, A. R., Cornia, P. B., et al. (2012). 2012 Infectious Diseases Society of America guidelines for the diagnosis and treatment of diabetic foot infections. Clinical Infectious Diseases, 39(7), 885-910.
[4] American Academy of Family Physicians. (2021, October). Diabetes-related foot infections: Diagnosis and treatment. American Family Physician, 104(4), 386-399. Retrieved from https://www.aafp.org/pubs/afp/issues/2021/1000/p386.html
[5] NCBI/NIH. (2025, April 10). Diabetic foot infections. StatPearls. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK441914/
[6] Satterfield, K., et al. (2023, July). Diabetic foot ulcers: A review. JAMA, 330(1), 62-75. Retrieved from https://pubmed.ncbi.nlm.nih.gov/37395769/
[7] Schmidt, M., PhD. Personal communication. (2025). Copper mechanisms in antimicrobial textiles. Medical University of South Carolina.
[8] Thieman, M., MD. (2025). Quantitative antimicrobial efficacy data: Copper-embedded textiles. West Virginia University Health System/VivoThreads Medical Director.
[9] SmarTex Yarn. Why choose copper ion antibacterial fiber for medical textiles. Retrieved from https://www.smartexyarn.com/blog/why-choose-antibacterial-copper-ion-fiber-for-medical-textiles/
[10] Nature. (2023, July 23). Antibacterial and biofilm-inhibiting cotton fabrics decorated with reduced graphene oxide and copper nanoparticles. Scientific Reports, 13, 12357. https://www.nature.com/articles/s41598-023-38723-4
[11] Facility-Level Variation in Major Leg Amputation Among Patients with Diabetic Foot Ulcers. (2025, April). JAMA, 333(17), 1668-1680. PMC12019509.